Celebrating Six Years of PCHSS Success: Research Showcase Highlights
On Friday 16th June 2023, researchers and other stakeholders gathered at Macquarie University for the PCHSS Research Showcase ‘Future proofing healthcare: what evidence tells us about creating sustainable healthcare systems’; there were over 60 in-person attendees and over 110 joining online. Not only was the event large in numbers, but also in scope: attendees included PCHSS researchers, other academics, individuals working at nationwide local health districts and external research centres, and industry professionals from companies such as Microsoft, KPMG and iCare. Such a range of attendees allowed for insightful, diverse perspectives to be heard throughout the day.
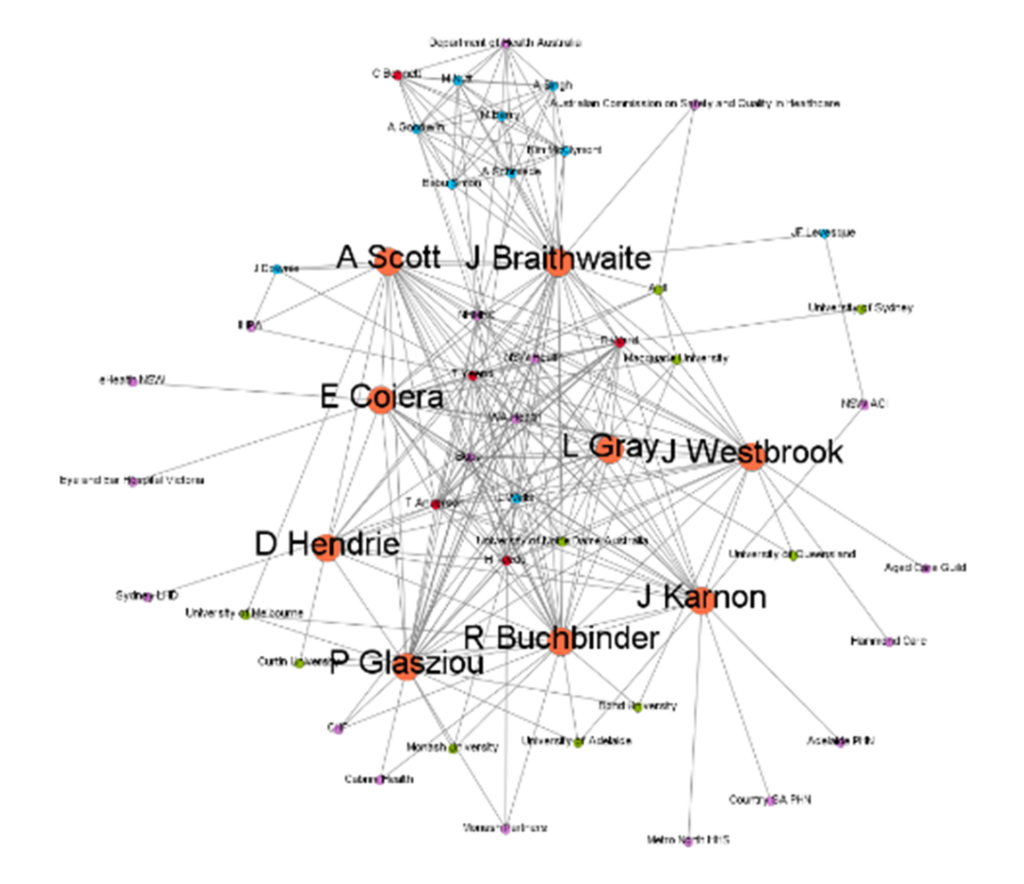
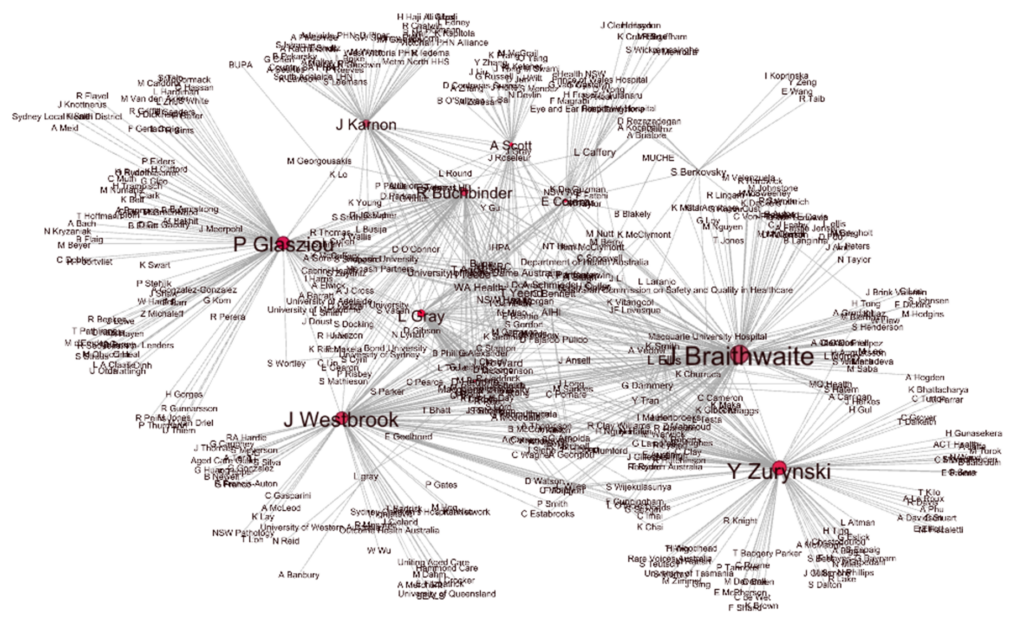
After an acknowledgement of country by Ms Carol Dixon of the Walanga Muru program at MQ Uni, Professor Jeffrey Braithwaite emphasised the growth and success of the PCHSS over the past 6 years. What started as a 10.75 million grant generated over $143 million in leveraged funding, and resulted in 867 peer-reviewed publications and reports. Over the past 6 years, the PCHSS network has grown substantially to include over 350 contributing authors, and we have conducted over 1000 conference presentations, webinars and reports.
We were joined by two special guests from NSW Health: Dr Jean-Frédéric Levesque, Deputy Secretary, Clinical Innovation and Research and Chief Executive, Agency for Clinical Innovation and Ms Deborah Willcox, Deputy Secretary, Health System Strategy and Patient Experience. Jean-Frédéric and Deb presented on how NSW Health are working to inform the sustainability of their health system, including models of care integration, managing gaps in prevention, and keeping an outcomes focus. Jean-Frédéric highlighted the need for alternate clinical trajectories, which look at efficiency within the health system and methods of strengthening it for the future. As one of the largest states in the Commonwealth, it was great to hear how NSW is leading the way.
“We believe the foundational work and the work of clinicians and researchers and all of our partners across the system are really setting us up well. We have a world class health system.”
Ms. Deborah Willcox
The next presenters were those from PCHSS Research Stream 1, Using Analytics, Technology and Shared Data. Professor Johanna Westbrook kicked this section off with a dazzling presentation that covered medication administration errors and double-checking, a process that costs one hospital around $2.7 million a year.
Professor Shlomo Berkovsky, who presented on behalf of Professor Enrico Coiera, also emphasised how big data can answer clinical questions by discussing their research that uses AI to produce refined data-driven clustering of frail patients, such as those with delirium and dementia. Dr Liam Caffery (on behalf of Professor Len Gray) reported on the great telehealth experiment, calling attention to how the use of telehealth has undoubtedly increased since the advent on COVID-19, but future uses could increase its potential. Like Johanna, Liam highlighted the need for collaboration with consumers to ensure that healthcare delivery is as efficient and effective as possible.
Professor Paul Glasziou AO and Professor Rachelle Buchbinder AO followed up with an engaging insight into Reducing Waste and Low-value Care (Research Stream 2). Drawing on audience participation and real-life case studies, both Professor Glasziou and Professor Buchbinder demonstrated the harm and waste that can result from definitional changes to conditions such as gestational diabetes, as well as from high use of imaging modalities. Not only does low-value care increase healthcare use and burden on services, but as Rachelle highlighted, MRI and CT machines also contribute substantially to carbon emissions and waste billions of dollars every year.
Promoting Better Value for the Health Dollar is the key focus of Research Stream 3. Professor Tony Scott highlighted that focusing on the architecture of the health system can help inform research into funding models, markets, competition and incentives, such as recommendations from the Medicare Benefits Schedule Review Taskforce. Professor Jon Karnon further broke down the bread and butter of health economics, emphasising that an embedded economic evaluation program has great potential to be used to further develop health systems and re-design services. Abby Mosedale also presented on behalf of Associate Professor Delia Hendrie, using the ‘trojan mouse’ principle to help explain the realist evaluations her team is conducting. It was fascinating to hear about the ways that economics and healthcare intersect.
Professor Yvonne Zurynski and Professor Jeffrey Braithwaite of the Observatory on Health System Sustainability (OHSS) closed the block of formal presentations. Professor Zurynski spoke about the increasing need for integrated care, explored through her KidsGPS, HeartConnect and Type 1 Diabetes Transition projects, and also gave insight into the Health Consumer Sentiment Survey conducted in collaboration with the Consumers Health Forum of Australia (CHF). Former CEO of CHF, Ms Leanne Wells, also spoke about the importance of involving consumers in research. Professor Braithwaite delivered a passionate talk about the need for health systems to adapt and prepare for future crises like pandemics and climate change, which can be developed by using the Learning Health System 2.0 approach. It was also fantastic to hear about the reach of the OHSS research, with connection to the World Health Organization, European Union, Harvard University, and the OECD.
After lunch, the health system simulation focused on a hypothetical scenario, in which stakeholders such as the treasury, health department, health workforce and corporate partners, were required to brainstorm solutions to the problem at hand. What was evident was that siloed decision-making within each stakeholder unit could only go so far; to solve the problem with the health system, groups needed to join forces and develop collaborative ideas.
It was an engaging activity, and in true simulation fashion, emphasised some of the key areas of improvement within the health system. For instance, collaboration with the health consumers group was minimal, which as discussed in a prior presentation by Ms Leanne Wells, is critical for the sustainability of the health system
Events such as these are not only a celebration of the Partnership Centre, but an opportunity for members of the community and other research partners to learn more about health system sustainability, and use that knowledge to shape the health system as we know it. While the research showcase symbolised the end of this era of the NHMRC PCHSS, the collaborations and connections that have been formed as part of the centre will continue into the future and we look forward to continuing to inform health system sustainability.




